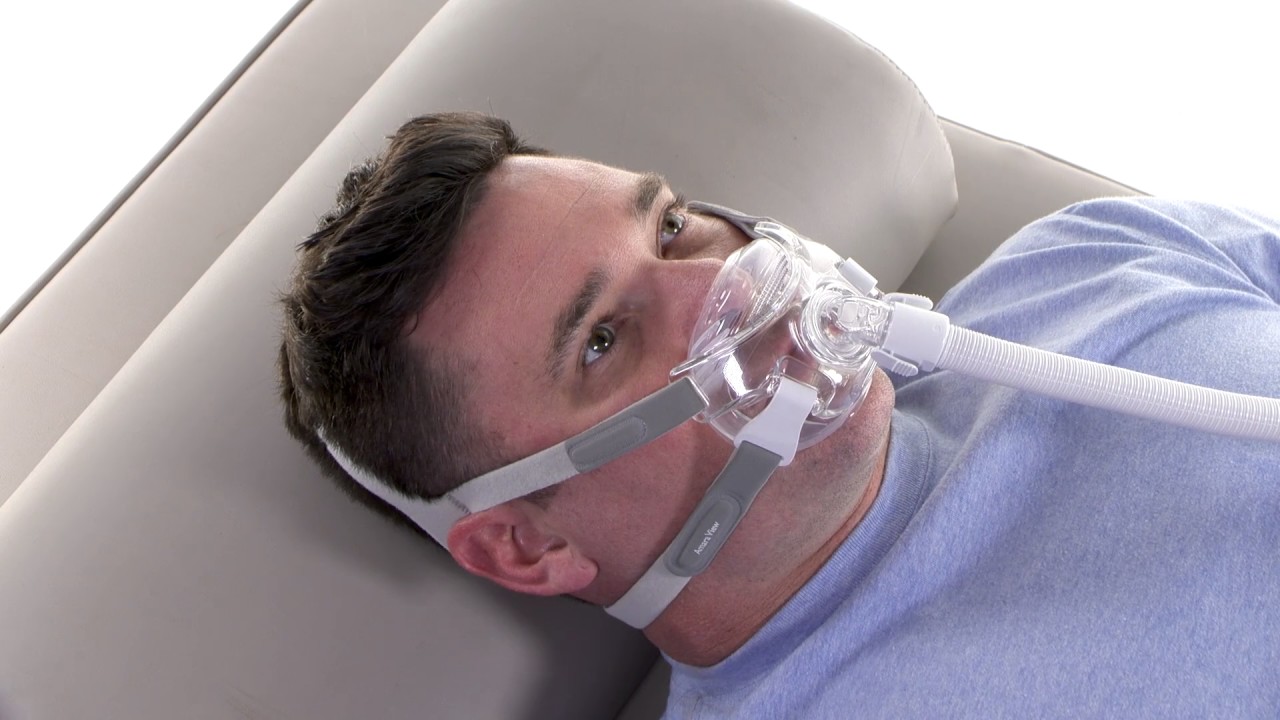
Tips for sleep apnea medical experts
As a sleep technologist, you often treat people who have sleep apnea. Continuous positive airway pressure, often known as CPAP, is an effective and well-liked treatment for sleep apnea. Patients with sleep apnea use the non-surgical technique to open up their airways while they are sleeping.
According to the National Sleep Foundation, the disease affects more than 18 million Australians. The fact that the community of sleep technologists is so acquainted with the CPAP problem should thus not be surprising. Another well-known truth is how crucial it is to encourage your patients to continue their medication.
In this article, we’ll examine the importance of CPAP adherence, the factors that make it difficult for patients to stick to treatment plans, and eight techniques you may use to help your sleep apnea patients utilize their CPAP more often.

Why Is CPAP Compliance So Vital?
According to a 2012 MedScape article, 50% of patients who get CPAP either quit using it or don’t follow their treatment plan. People with sleep apnea must adhere to CPAP treatment diligently because if it is stopped, the ailment swiftly returns.
A tiny, randomized trial found that hourly arousal incidences had more than doubled after only two weeks without CPAP. According to a 2011 article in MedPage Today, the prevalence of apnea-hypopnea has increased by a factor of 17.
Objective sleepiness assessments did not significantly change, despite the fact that subjective tiredness and OSA returned a few days after the CPAP treatment finished. By the end of the experiment, endothelial function was much worse than in those using CPAP, and morning heart rate, blood pressure, and urine catecholamine levels were all significantly increased.
You can see that patients must strictly adhere to their treatment plan in order to maintain their health.
Why Is CPAP Adherence in Patients So Difficult?
A patient’s CPAP tolerance and adherence may suffer from a variety of pressure, patient, and mask-related issues. Knowing the most common sleep apnea signs and problems can help you as a sleep technician identify potential nonadherence concerns.
As our article, Top 10 Most Common CPAP Mask Problems and Discomfort (& How to Solve Them), demonstrates, there are a number of common issues with treatment. These consist of:
- An unease with using the CPAP mask and a difficulty getting used to it.
- Worrying that their mask would cause an allergy.
- Not being able to tolerate the forced air from the mask.
- Having a runny or stuffy nose after using a CPAP machine.
- A tightening sensation when wearing the mask.
- Sleeping difficulties while using a CPAP machine.
- Having a dry mouth after putting on the mask.
- Frequently removing their sleep mask.
- Being unable to stand the machine’s noise.
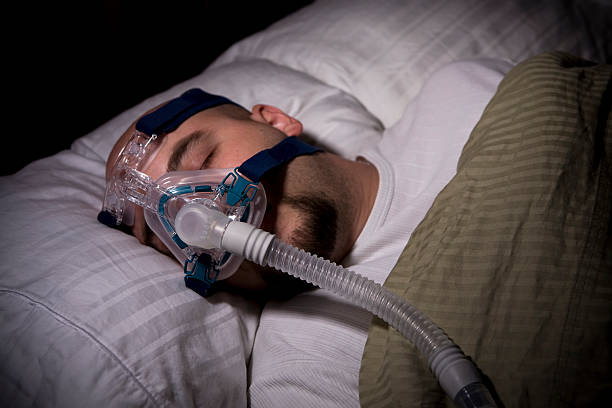
Any of the aforementioned issues might lead to new CPAP users stopping their treatment suddenly. This underscores the importance of discussing potential CPAP difficulties and solutions with your patients.
What steps can sleep researchers take to improve CPAP compliance?
It’s crucial for sleep technicians to provide patients the resources, information, and support they need to feel comfortable using CPAP treatment and, as a consequence, boost adherence. Take the following steps to achieve this: Educate Patients Before Treatment (And Continuing Throughout Treatment)
Make sure your patient understands all of the CPAP machine’s characteristics, the therapy it offers, any possible issues, and how it will help them with their sleep apnea symptoms before giving them the CPAP mask. Tell them how to handle each common objection and how to prepare for them all.
Make sure they understand the risks of stopping their medicine and that, despite their early pain, they will gradually become used to it. Untreated sleep apnea has a detrimental effect on a patient’s health and quality of life, and you should make sure your patients are aware of this. Discuss any medical conditions that are said to exist or are known to exist. They may be more inclined to accept their treatment plan and, as a consequence, take more control over their health.
The early stages of therapy are when treatment cessation occurs most often. The CPAP mask may feel incredibly weird when first worn. It is advised that you explain to patients the effectiveness and benefits of CPAP therapy. This could motivate individuals to keep up their treatment throughout the first stages of the transition.

Finding the Right Mask Takes Time
For many individuals, wearing the improper mask results in issues. Giving your patient all of their options up front might increase adherence since, often, patients are reluctant to try another mask-type treatment after a bad experience.
There are three main types of masks:
Nasal pillows
These are situated under the nose, close to the nostrils’ entrance. Patients who wear glasses may utilize nasal pillows without having their eyesight blocked.
Masks that hide the face
Lips and the nose are enclosed by full-face masks. They are a good alternative for those who breathe through their lips.
Nasal shields
Nasal masks, which cover the nose, are more compact and lightweight than full-face masks. Additionally, they provide greater security than a nasal cushion.
Make sure to go through the benefits and drawbacks of each kind so that your patients will know which mask is best for them.
Consistent Check-Ins & Support Services
Make sure you often ask new CPAP users how they feel about the treatment and keep track of their adherence so that, in the event that it starts to fall, you can address any problematic behaviors as soon as possible.
It could seem strange and baffling to have to wear a mask every night in order to sleep. Numerous changes are occurring in the health of your patients. By being there for them and empathetic, you can ensure that they feel as comfortable as possible during their treatment. Kids will also find it easier to speak to you about problems or difficulties if they do have them.
Start Small
Do not immediately demand that new CPAP users who are having trouble adhering to the sleep apnea therapy wear the mask all night. Encourage them to wear the mask for a little bit longer each night to ease them into it. Set them small, manageable goals as they get closer to wearing the mask all the time. For instance, kids could practice putting on their mask while they are still awake.
First, they may put the mask over their faces without fastening it. Once they are comfortable, they could try putting the straps and the mask on. They can test holding the mask against their faces with the hose connected after turning on the ramp function and choosing the low-pressure setting on the device. They have to do this when they are awake. Once they feel comfortable enough, they might try sleeping with the mask on.

Do you experience any of these?
A Snoring History Many individuals snore, however not all snorers have sleep apnea. Some individuals only sometimes snore, such as after a few beers or a few glasses of wine. That isn’t really unusual. But the majority of those who suffer sleep apnea snore. As a result, it often serves as a sign of the illness. Pathological snoring may be distinguished from regular snoring by a few factors, including: the level of force, volume, and frequency. Snoring is most likely not a symptom of a health problem if it just occurs sometimes. It is far more likely that you have sleep apnea if you snore loudly every night. Because it is so loud, some physicians refer to the snoring linked to sleep apnea as “destructive snoring.”
Dr. Malhotra said, “I’ve had patients whose children are on a separate story of the home and they can still hear them snoring.” “I’ve had patients whose next-door neighbors would complain about their snoring,”
Daytime sleepiness: You may have sleep apnea if you need many cups of coffee merely to get through the day. People with it regularly wake up in the middle of the night by their interrupted breathing, which causes them to fall asleep at inappropriate times and places, such as when driving or working.
Dr. Malhotra observed that while many individuals claim they are not drowsy throughout the day, the amount of coffee they consume is substantial. Even though tiredness is a typical symptom, many individuals who are caffeine-pumped don’t fall asleep at inappropriate times.
Witness Apnea: Some individuals with sleep apnea are only made aware of it by their spouses. It is known as “witness apnea” by doctors. According to Dr. Kryger, “a typical reason individuals are referred is because their bed partner is afraid—not of the snoring, but of the stillness in between it. It’s absolutely scary. It suggests that they are genuinely ceasing to breathe. When others see it, they often say things like, “My God, something is wrong with this individual. They can’t breathe,’
Obstructive Sleep Apnea and High Blood Pressure: This relationship between the two conditions is well-known. According to some professionals, the connection is reciprocal: You are more likely to develop high blood pressure if you have sleep apnea, and high blood pressure exacerbates the condition. It’s a risky cycle. Because of how closely related the two are, there is a strong likelihood that if you have hypertension, you also have sleep apnea. Hypertension affects more than half of all sufferers of severe sleep apnea. Additionally, sleep apnea is more common than 80% among persons with resistant hypertension, meaning their blood pressure stays high after taking various medicines. The bottom line: Sleep apnea may also exist if you have excessive blood pressure.
Other indications that you may have sleep apnea include:
- Sleep issues or recurring awakenings
- a painful throat upon waking; frequent morning headaches; and drowsiness throughout the day. Having trouble focusing Forgetfulness.
Have it examined
The most crucial action you should take if you think you may have sleep apnea is to see a specialist. Talk to a sleep medicine expert or your health care physician about your symptoms. A sleep test, which may be completed either at home or in a lab, will probably be scheduled for you by your doctor.
For the standard sleep test, also known as a polysomnogram, you must spend the night in a sleep lab. There, you’ll be connected to a number of devices that monitor and record your heart rate, respiration, blood oxygen levels, and brain waves as you sleep. You will be asked to return to the lab a second time if the study reveals that you have sleep apnea so that you can be fitted for a CPAP machine, or continuous positive airway pressure, which gently blows air into your airway at night to keep it open.
